Long-Term Concussion Effects, Treatment & More
Concussions can have long-term physical, cognitive, and emotional effects. Symptoms such as brain fog, headaches, and depression can last for months or years after the initial injury. When the...

Concussions may be the hardest form of traumatic brain injury to treat due to the convoluted nature of long-term symptoms and how those symptoms can be misdiagnosed or even undiagnosed.
15 to 20% of those injured with a mTBI develop symptoms meeting criteria for psychiatric disease including PTSD, anxiety, panic disorder, OCD, and depression. Recent studies have also found a connection between increased risk of suicidality and head injuries.
Medications are often prescribed by a multitude of different clinicians to treat these types of symptoms, but the first concern is always whether or not the medications are appropriate for the patient.
This problem becomes even more concerning as we see more patients who have been prescribed with several seizure medications, sleep aids, and psychiatric drugs. Often the side effects of these medications can mimic or even exacerbate the concussion symptoms we are trying to resolve.
Thus starts a complicated Symptom-Medication-Exacerbation Cycle (SME Cycle). The more you continue the cycle the more symptoms increase or continue and medications get perscribed.
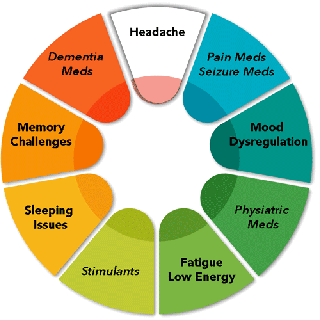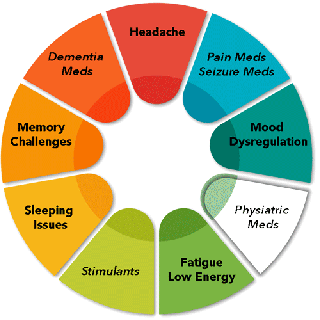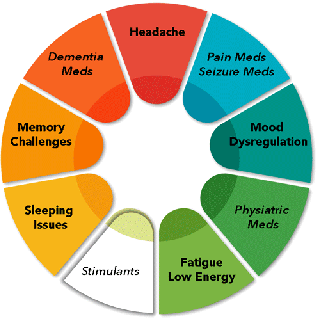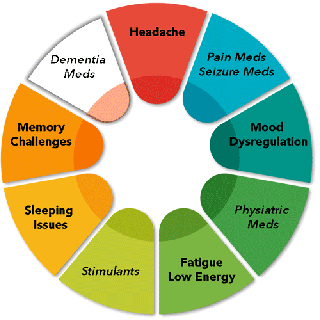
Here is a table of common medications used for a concussion, along with their common side effects, that can influence the SME cycle:
| Drug | Condition Being Treated | Side Effects |
| Lamictal | Seizures | Insomnia, drowsiness, fatigue, dizziness, anxiety, pain, irritability, suicidal ideation, abnormal dreams, abnormality in thinking, agitation, amnesia, depression, emotional lability, hypoesthesia, migraine, confusion |
| Amitriptyline |
Headaches, Depression, Fatigue, Insomnia |
Sedation, impaired memory, delirium, hallucinations, convulsions, coma, cardiotoxicity |
| Propranolol |
Migraines |
Agitation, fatigue, dizziness |
| Sertraline |
Depression and PTSD |
Insomnia, headache, dizziness, fatigue |
| Citalopram |
Depression, Anxiety, PTSD, Panic and Social Anxiety |
Drowsiness, insomnia |
| SSRI's |
Depression and PTSD |
Insomnia, headache, dizziness, fatigue, SIADH |
| SNRI's |
PTSD and Depression |
Elevated blood pressure, stimulant, agitation, neuromuscular activity decline |
| Antipsychotics |
Mood Disorder and PTSD |
Gyencomastia, dyskinesia, sedation, hyoptension |
| Carbamazepine |
Mood Stabilizer |
Agranulocytosis, diplopia, ataxia |
If you are currently taking any of these and noticing that you aren’t feeling better, the above cycle may explain why. It is critical to recognize that if you have had a concussion or traumatic brain injury, this fact can be contributing to the cause of your symptoms. Please be open to talking to your doctor about reducing the medications, if possible.
Using medications to treat a concussion or the effects of a concussion may be helpful in the short-term to mask some symptoms, but may not be an effective long-term solution. Please inform yourself about these medications and their side effects. Your doctor is your advocate and trying to find you relief; however, he or she may not always be aware of the long-term effects of the medications psychologically and how these meds may actually be inhibiting your brain from healing.
One of our goals is to help our patients need as few medications as possible so that we can get to the core problem of the brain injury, thus helping the brain readjust and recover without the need for multiple medications.
The goal is always to restore brain function to its fullest potential. Each injury and each person will heal differently, which is why we take a targeted and individualized approach to get to the bottom of the symptoms.

Dr. Alina K. Fong received her Ph. D. in Clinical Neuropsychology with an emphasis in neuroradiology from Brigham Young University. She received the national American Psychological Association Clinical Neuropsychology Division 40 Graduate Student Research Award in 2004 for her research on "Cortical Sources of the N400 and 'The N400 Effect." Dr. Fong's interest in brain mapping soon turned to functional MRI, and since then, her research efforts have been focused on the clinical applications of fMRI.

Concussions can have long-term physical, cognitive, and emotional effects. Symptoms such as brain fog, headaches, and depression can last for months or years after the initial injury. When the...
A concussion is a traumatic brain injury (TBI) which is caused by the brain hitting the skull. This can happen in sports, car accidents, falling, or anything similar. A concussion can even be the...